Colic and the Nervous System: Why Your Baby Can't Stop Crying
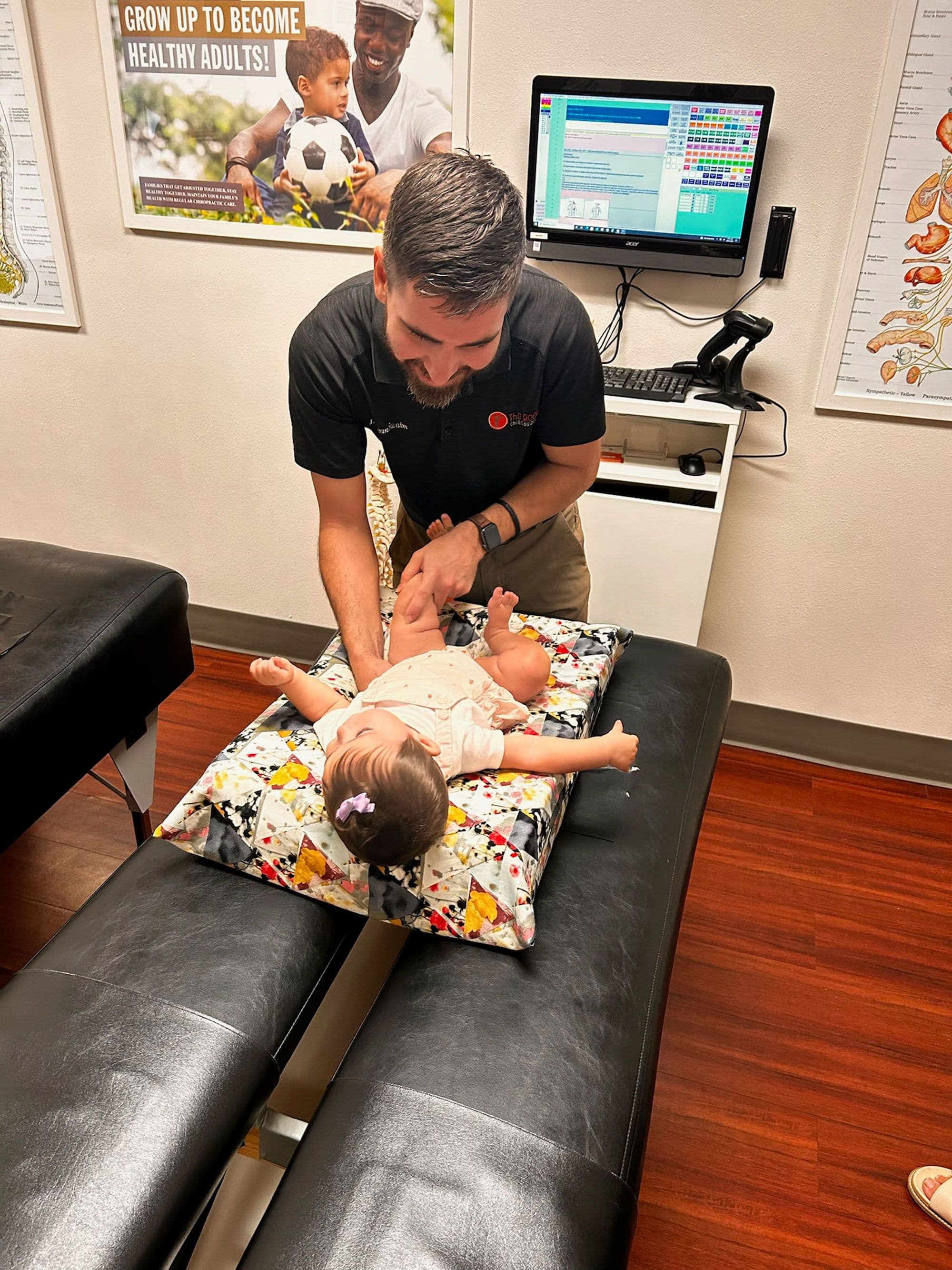
Your baby screams for hours. Back arched, fists clenched, face red. You've fed them, changed them, held them, bounced them, driven around the block at 2 a.m. Nothing works. Your pediatrician says it's colic — and that they'll grow out of it.
That last part might be true. But "wait it out" isn't a plan. And what most parents never hear is that colic is often a nervous system problem, not a stomach problem.
What Colic Actually Is (and Isn't)
The medical definition of colic is crying for more than three hours a day, more than three days a week, for more than three weeks — in an otherwise healthy baby. That's called the Wessel criteria, and it's been the standard since 1954.
Here's the problem with that definition: it describes the symptom without touching the cause. It tells you your baby cries a lot. It doesn't tell you why.
Colic is not a diagnosis. It's a label for a pattern of distress that nobody has explained yet. And for decades, the default explanation has been "immature digestive system" or "gas." But a growing body of research points somewhere else entirely — the autonomic nervous system.
The Nervous System Connection Most Parents Miss
Your baby's autonomic nervous system has two modes:
- Sympathetic — the stress response. Fight or flight. Heart rate up, digestion slowed, muscles tense.
- Parasympathetic — the calm response. Rest and digest. Heart rate down, digestion active, muscles relaxed.
A healthy newborn moves fluidly between these two states. A colicky baby gets stuck in sympathetic dominance — locked in a stress response they can't turn off on their own.
When the nervous system is stuck in sympathetic mode, here's what happens downstream:
- Digestive motility slows. Food moves through the gut slower, causing gas, bloating, and discomfort.
- The gut-brain axis fires incorrectly. Signals between the brain and the digestive system become disorganized.
- Muscle tension increases. That classic colic posture — arched back, clenched fists, drawn-up knees — is a physical expression of nervous system tension, not just pain.
- Sleep regulation breaks. A baby stuck in fight-or-flight struggles to settle into deep, restorative sleep cycles. (This is why colic and sleep issues so often travel together.)
The crying isn't random. It's your baby's nervous system telling you it's overwhelmed and can't self-regulate.
Why Birth Is the Starting Point
Most colic cases we see at Little Roots trace back to what happened during birth. Even a straightforward vaginal delivery puts significant mechanical stress on a newborn's spine and cranium:
- Compression through the birth canal
- Rotation of the head and neck during crowning
- Traction — pulling forces applied to the head and neck as baby emerges
When birth involves intervention — vacuum extraction, forceps, prolonged pushing, emergency C-section — those forces increase substantially. Research published in the Journal of Manipulative and Physiological Therapeutics has documented that routine deliveries can apply forces to the infant cervical spine that would be considered excessive in an adult context.
The result: subtle misalignments in the upper cervical spine and cranium that interfere with how the vagus nerve communicates between the brain and the gut. The vagus nerve is the primary parasympathetic pathway — when it's compressed or irritated, the baby's ability to shift into "rest and digest" mode is compromised.
That's colic. Not a bad stomach. A nervous system that can't downshift.
What Colicky Babies Actually Look Like in Our Office
Parents bring their babies to Little Roots when they've tried everything else — gas drops, different formulas, elimination diets, white noise machines, specific holds. Some of it helps a little. None of it resolves the pattern.
The common presentations we see alongside colic:
- Reflux — frequent spit-up, arching during or after feeds, refusing the breast or bottle
- Latching difficulty — baby can't maintain a deep latch, clicks while nursing, favors one side
- Head turn preference — baby consistently turns their head one direction, won't look the other way
- Fussy at specific times — late afternoon and evening meltdowns (when the nervous system is most depleted)
- Sleep disruption — waking constantly, never settling into long stretches, only sleeping when held upright
When multiple symptoms cluster together like this, it's not five separate problems. It's one nervous system under stress expressing itself in different ways.
How Pediatric Chiropractic Care Helps
Pediatric chiropractic for colic is not about "cracking a baby's back." The adjustment used on a newborn involves fingertip pressure roughly equivalent to what you'd use to test whether a tomato is ripe. Most babies sleep through it.
At Little Roots, we use Torque Release Technique — an instrument-assisted method that delivers a precise, low-force impulse to specific areas of the spine where nerve interference is detected. No twisting. No popping. No manual thrusting.
Here's what gentle spinal care does for a colicky baby:
Releases the vagus nerve pathway. When subtle misalignments in the upper cervical spine are corrected, the vagus nerve can communicate freely between the brainstem and the digestive system. Parasympathetic function improves. Digestion normalizes.
Shifts the nervous system out of sympathetic dominance. The adjustment gives the nervous system permission to downregulate — to move from fight-or-flight back into rest-and-digest. Parents often describe the shift as "getting their baby back."
Reduces global muscle tension. That arched back and those clenched fists soften. Baby's body relaxes because the neurological driver of the tension has been addressed.
Improves sleep regulation. A nervous system that can self-regulate transitions into sleep more easily and stays asleep longer. This is consistently the first change parents notice.
What the Research Says
A 2012 systematic review in the Journal of Manipulative and Physiological Therapeutics analyzed multiple studies on chiropractic care for infantile colic and found significant reductions in crying time compared to control groups. A separate 2014 study in the journal Chiropractic & Manual Therapies examined over 2,000 infant patients and reported that adverse events from pediatric chiropractic care were rare and mild — primarily limited to brief fussiness.
The evidence base is growing, though most studies are observational rather than randomized controlled (RCTs in infant populations are ethically and logistically difficult to design). The clinical consensus among pediatric chiropractors is that gentle spinal care is safe and meaningfully helpful for many colicky infants.
For a deeper look at the safety question, read Is Chiropractic Safe for Babies?
What a First Visit Looks Like
Your first visit at Little Roots includes:
- A thorough history — pregnancy, birth details, feeding patterns, sleep, crying patterns, what you've already tried
- A gentle hands-on evaluation — baby on your lap or a padded table. We assess cranial motion, cervical mobility, sacral alignment, and tension patterns
- A neurological evaluation — non-invasive scans that show us how your baby's nervous system is functioning right now
- If indicated, a gentle adjustment — your doctor demonstrates the Integrator instrument on your hand first so you feel exactly how light the force is before touching your baby
The entire visit takes 15–20 minutes. Most babies are calm or sleeping by the end.
Each child is different. We take a personalized approach based on what your child's nervous system is showing us — never a one-size-fits-all protocol.
When to Bring Your Baby In
The earlier, the better. The held-tension patterns from birth are most responsive to gentle correction in the first weeks and months of life. If your baby is showing any combination of:
- Inconsolable crying episodes lasting hours
- Back arching during feeds or crying
- Difficulty latching or nursing on one side
- Disrupted sleep despite being well-fed and dry
- Visible discomfort with gas or bowel movements
- Head tilt or strong turn preference
Don't wait for them to "grow out of it." The nervous system patterns driving colic don't always resolve on their own — and the sooner they're addressed, the easier the correction.
Frequently Asked Questions
How quickly do babies respond to chiropractic care for colic?
Many parents notice a shift within the first few visits — calmer feeding, longer sleep stretches, less intense crying episodes. Every baby responds differently, and we track progress with periodic re-evaluations rather than promising specific timelines.
Is chiropractic safe for a newborn?
Yes. Pediatric chiropractic uses fingertip pressure lighter than you'd use to check a ripe tomato. It is gentle enough that most babies sleep through their adjustment. Our doctors are trained specifically in infant and pediatric care — including ICPA and PX certifications.
Can colic be caused by food sensitivities?
It can be a contributing factor, but it's rarely the whole picture. Many parents try elimination diets and formula changes without full resolution — because the underlying nervous system tension remains. Addressing both the dietary and neurological components together tends to produce the best outcomes.
Should I still see my pediatrician about colic?
Absolutely. Chiropractic care does not replace your pediatrician. We encourage every family to maintain regular well-child visits. Pediatric chiropractic addresses a specific gap — the mechanical and neurological consequences of birth — that conventional pediatrics isn't designed to evaluate.
Do I need a referral to bring my baby in?
No referral is needed. You can book a free newborn check directly or call (941) 932-4611 to schedule.
How many visits will my baby need?
Each child is different. We take a personalized approach based on what your baby's nervous system is showing us. We never commit to a set number of visits upfront — progress re-evaluations guide the care plan as your baby responds.
Colic is real. The exhaustion is real. And the frustration of hearing "they'll grow out of it" when your baby is screaming in your arms at 3 a.m. is real.
But colic is not a personality. It's not a phase you just survive. In many cases, it's a nervous system that got stuck during birth and needs a gentle hand to help it regulate.
If that sounds like your baby, the Little Roots team would love to meet your family. Book a free newborn check or call (941) 932-4611.
Conditions We Treat
Colic
Colic isn't a personality trait — it's often a baby's nervous system stuck on high alert. Gentle chiropractic care helps the system downshift so feeding, sleeping, and being held start to feel okay again.
Reflux
Spit-up is normal. Arching through feeds, crying after eating, sleeping fitfully, and never seeming satisfied — that's reflux, and it's almost always a nervous-system regulation story before it's a digestion story.
Sleep Regulation
Short naps, frequent wakings, a baby or toddler who fights sleep no matter what you try — these are signals that the nervous system is stuck in 'on.' Gentle care helps it find the off switch.
